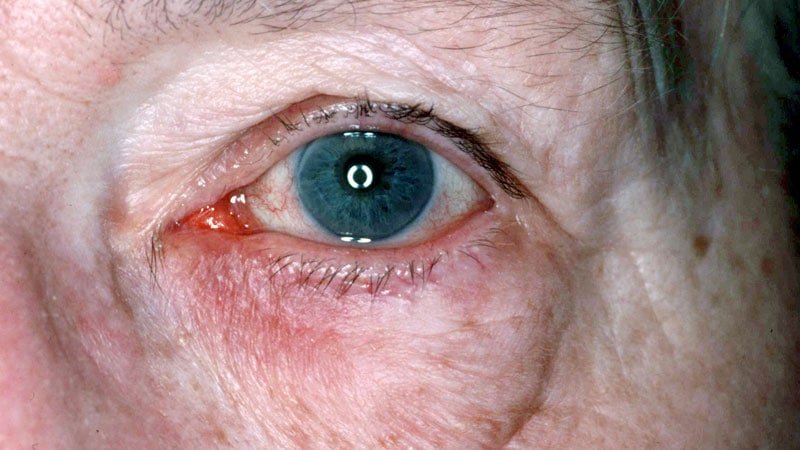
Patients with rosacea are more likely to experience ocular symptoms, including foreign body sensations, itching, dryness, hyperemia, and conjunctival telangiectasia, according to a study recently published in International Ophthalmology.
In the study, investigators compared the right eyes of 76 patients with acne rosacea and 113 age-matched and gender-matched patients without rosacea. The mean age of the patients was 47 to 48 years, and about 63% were females. Ophthalmologic examinations that included tear breakup time and optical coherence tomography–assisted infrared meibography were conducted, and participants were asked to complete the Ocular Surface Disease Index (OSDI) questionnaire, which the authors say is widely used to assess aspects of ocular surface diseases.
Compared with controls, significantly more patients with rosacea had itching (35.5% vs 17.7%), dryness (46.1% vs 10.6%), hyperemia (10.5% vs 2.7%), conjunctival telangiectasia (26.3% vs 1.8%), and meibomitis (52.6% vs 31%) (P ≤ .05 for all), according to the investigators, from the Departments of Ophthalmology and Dermatology, Dokuz Eylul University School of Medicine, Izmir, Turkey. The most common ocular symptom among those with rosacea was having a foreign body sensation (53.9% vs 24.8%, P < .001).
Ocular surface problems were also more common among those with rosacea, and OSDI scores were significantly higher among those with rosacea, compared with controls.
Estee Williams MD, a dermatologist in private practice in New York City and assistant clinical professor of dermatology at Mount Sinai Hospital, who was not involved with the study, said the results reinforce the need to keep ocular rosacea in mind when examining a patient.
“The study is a reminder that ocular rosacea is, like its facial counterpart, an inflammatory disease that can manifest in many ways; for this reason, it’s often misdiagnosed or missed altogether,” Williams told Medscape Medical News. “This is unfortunate because it is usually easily managed.”
She added that there is a need for more randomized, controlled studies to determine optimal treatments for ocular rosacea, which is underdiagnosed. Part of the reason she believes it is underdiagnosed is that often, “ophthalmologists don’t think about ocular rosacea specifically, unless they are given the information that the patient suffers from rosacea. The patient may not be aware that their skin and eye problems are connected.”
The take-home message of the study, Williams added, is that dermatologists who treat rosacea should be ready to screen their patients with rosacea for ocular symptoms, as well as have a basic understanding of ocular rosacea and know when to refer patients to an ophthalmologist.
“Preservative-free eyedrops are usually well tolerated and a good starting point for those cases that are limited to symptoms only,” she said. “However, once a patient has signs of overt inflammation on exam, such as arcades of blood vessels on the eyelid margin or on the white of the eye, prescription medication is usually needed.”
A limitation of the study is that both eyes of patients were not included, said Williams, noting that ocular rosacea is usually bilateral.
Also asked to comment on the results, Marc Lupin, MD, a dermatologist in Victoria, British Columbia, Canada, and clinical instructor in the Department of Dermatology and Skin Science, University of British Columbia, Vancouver, noted that one of the shortcomings of the study is that it did not account for any effect of treatment.
“Were they on treatment for their rosacea either during the study or before the study?” asked Lupin. “That would affect the ocular findings.” Still, he agreed that the study underlines the need for dermatologists to be aware of the high incidence of ocular rosacea in patients and to appreciate that it can present subtly.
The study authors, Williams, and Lupin have disclosed no relevant financial relationships.
Int Ophthalmol. Published online November 2, 2021. Abstract
For more news, follow Medscape on Facebook, Twitter, Instagram, and YouTube.
Source: Read Full Article