Coronary Artery Disease (CAD) is the most common form of heart disease, accounting for about 20% of local deaths. Recent studies by NHCS looked into data that are unique to the Asian population and discovered two distinct methods which can potentially improve the prediction of CAD in our local community. The results were published in the Journal of the American Heart Association.
Multi-center study develops patented novel analytical method for local community
Generally, patients suspected to have CAD will undergo several diagnostic tests to accurately diagnose the disease, including an invasive coronary angiogram (ICA) which is the current gold standard in assessing and diagnosing CAD. ICA involves injecting dye (contrast material) into the patient and then using X-rays to see how blood flows through the coronary arteries. During ICA, fractional flow reserve (FFR) is used to measure blood pressure within a coronary artery, which can determine the functional significance of coronary artery stenosis (i.e. the degree of narrowing of the coronary artery influences blood flow and can lead to a heart attack).
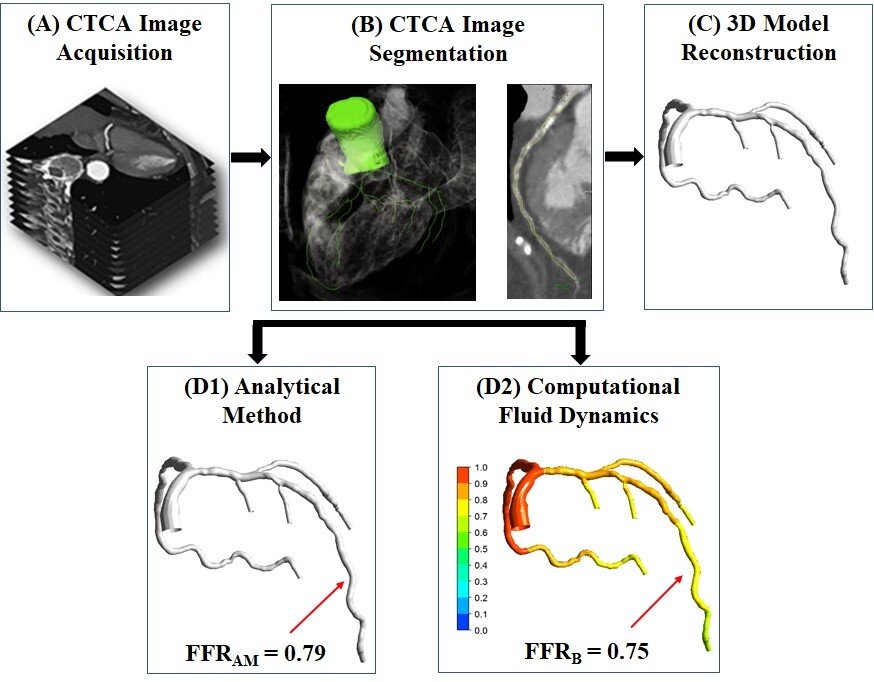
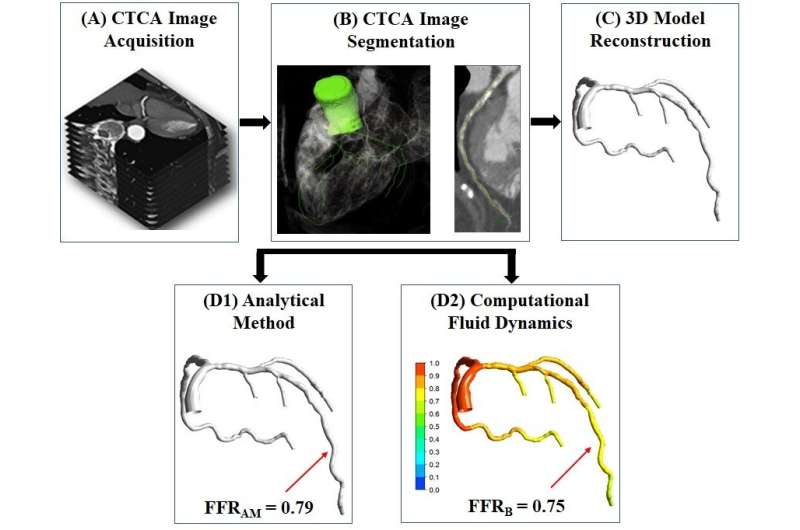
Over 100 patients who had undergone non-invasive CT coronary angiogram (CTCA), ICA and invasive FFR were recruited in this multi-center research study. Led by Associate Professor Zhong Liang, Principal Investigator, National Heart Research Institute Singapore (NHRIS), NHCS, the team experimented a novel analytical method of measuring blood pressure within a coronary artery—using 3-dimensional (3D) models reconstructed from these patients’ CTCA images, and analyzed the data of both the invasive and non-invasive tests.
“Through the study, we demonstrated that this novel analytic method from non-invasive CTCA images and computational method, delivers comparable accuracy of determining the blood pressure within the coronary arteries, to current invasive diagnostic tests. This could potentially reduce invasive angiography, enhance patient safety and management as patients can opt for this non-invasive method instead,” said Assoc Prof Zhong Liang.
This novel method has been granted a patent by the United States Patent and Trademark Office and is currently undergoing further trial for potential clinical application in the near future.
Improved pre-test probability model tailored to mixed Asian population
Chest pain is a common symptom presented in patients with stable CAD. A guideline-recommended pre-test probability (PTP) score is a tool used by doctors to assess stable chest pain and guide their decisions on the next appropriate test and further management of the patient. The US and European guidelines recommend the use of various models and a variety of PTP scores such as the CAD Consortium 2 (CAD2) model.
Computerized Tomography (CT)-based coronary artery calcium scores measure the amount of calcium in the arteries (built-up plaque) and is a well-established predictor of the likelihood of CAD and risk of future heart attacks. It is included in recent PTP scores validated for the Western population.
“As the guidelines are validated for the Western population, the performance of these tools may vary when applied to the local Asian population due to differing ethnic group compositions and geographical locations,” said Dr. Lohendran Baskaran, Senior Consultant, NHCS. “Some studies have shown these scores tend to overestimate the prediction of CAD in Asians leading to unnecessary investigations and treatments.”
Therefore, the research study led by Dr. Baskaran aimed to evaluate the effectiveness of the PTP score, specifically the CAD2 model as well as the inclusion of CT-based coronary artery calcium scores in predicting obstructive CAD in patients with stable chest pain in a mixed ethnic cohort in Singapore. The study which analyzed over 500 patients’ scores for CAD showed that the incorporation of CT-based coronary artery calcium scores in the CAD2 model significantly improved the prediction of CAD. Tailored calibration to the local population further enhanced the model’s performance.
Source: Read Full Article