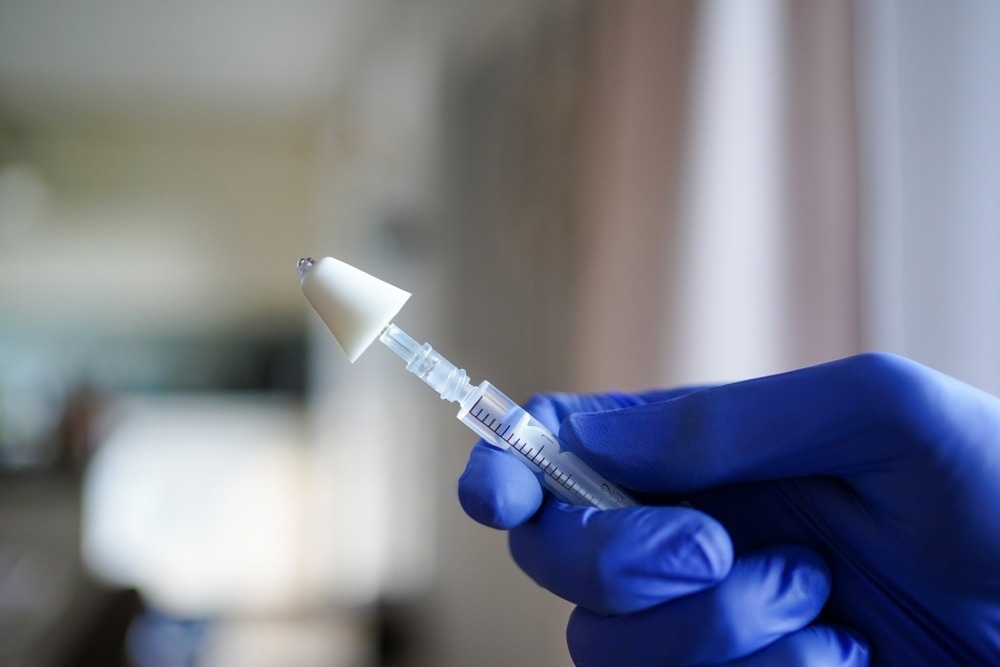
In a recent study published in Clinical Infectious Diseases, a team of researchers measured the antibodies against severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) from nasal fluid, saliva, and plasma to compare the antibody levels between blood and mucosal fluids.
Background
SARS-CoV-2 is known to enter the body through mucosal surfaces such as the nasal passages. However, most studies examining the level of protection against SARS-CoV-2 infections have measured the antibody levels in blood samples, and few have evaluated the antibody levels in mucosal fluids such as nasal secretions.
Given that SARS-CoV-2 infections largely occur in mucosal tissue, the antibody levels in nasal fluids and saliva might not correlate with those in blood. Furthermore, the antibodies in the mucosa could result from antibody transudation from the plasma or the production of antibodies by plasma cells in the mucosa. Determining the differences in antibody levels in mucosal fluids and blood could aid the development of mucosal vaccines against SARS-CoV-2.
About the study
In the present study, the team longitudinally measured the antibody levels in the nasal fluid, saliva, and plasma of individuals infected with SARS-CoV-2 before and after vaccination and vaccinated individuals who had not been infected with SARS-CoV-2. The participants comprised healthcare workers and other employees at the National Institutes of Health in Bethesda, Maryland, in the United States. The study was conducted between April 2020 and February 2022.
Blood samples were collected monthly from healthcare workers who came in contact with patients. Nasal fluid and saliva samples were also collected from the participants. The luciferase immunoprecipitation systems (LIPS) assay was performed to measure the anti-SARS-CoV-2 spike and nucleocapsid antibodies. Since immunoglobulin A (IgA) antibodies play an important role in mucosal immunity, IgA-specific antibody levels were also measured in the nasal fluid and saliva samples.
Results
The results reported that the levels of anti-nucleocapsid antibodies against SARS-CoV-2 declined faster than the anti-spike protein antibodies in the plasma samples of unvaccinated infected individuals. Vaccination increased the anti-spike antibody levels in the plasma, while the level of anti-nucleocapsid antibodies remained the same. The anti-spike antibody levels in the nasal fluid decreased faster than in plasma.
In vaccinated individuals who were not infected with SARS-CoV-2, the anti-spike antibodies in nasal fluid and saliva and the IgA-specific antibodies in the nasal fluid decreased faster than those in plasma. Furthermore, the increase in antibody levels after vaccination in individuals with previous SARS-CoV-2 infections varied across the plasma, saliva, and nasal fluid samples. While one vaccine dose resulted in a 22.4-fold increase in anti-spike antibodies in plasma, nasal fluid and saliva only exhibited an increase of 14.1 and 12.3-fold, respectively.
In unvaccinated, infected individuals, the anti-spike antibody levels in the nasal fluids and saliva correlated with that in the plasma, while the anti-nucleocapsid antibody levels did not, suggesting that the mucosal antibodies were most likely a result of transudation from plasma and were not produced by plasma cells in the mucosa. The authors believe that the rapid decline of mucosal antibody levels after the second vaccine dose as compared to the antibody levels in plasma might explain the increase in breakthrough infections despite high antibody levels in the blood.
Furthermore, intramuscular administration of the SARS-CoV-2 vaccine might be responsible for the lower and short-lived antibody levels in mucosal tissue. Vaccines given through the oral or intranasal route might produce stronger mucosal immunity against SARS-CoV-2. Oral poliovirus vaccines and intranasal influenza vaccines have shown better protection against disease than intramuscularly administered vaccines.
Furthermore, experiments with animal models have shown that intranasal vaccinations against SARS-CoV-2, as well as SARS-CoV-1 and Middle East respiratory syndrome (MERS), have been more effective than intramuscular vaccines.
Conclusions
To summarize, the study measured the antibodies against SARS-CoV-2 spike and nucleocapsid proteins in plasma, saliva, and nasal fluid samples of individuals infected with SARS-CoV-2 before and after vaccinations, as well as SARS-CoV-2-naive, vaccinated individuals.
The results suggested that in unvaccinated, infected individuals, the anti-spike antibody levels in nasal fluid and saliva correlated with that in plasma, indicating the transudation of antibodies from blood to mucosa. Anti-nucleocapsid antibody levels in saliva, nasal fluid, and plasma declined rapidly compared to anti-spike antibody levels.
Furthermore, vaccinations did not boost the antibody levels in nasal fluids and saliva to the same extent as in plasma, suggesting that intramuscularly administered vaccines might not be effective in increasing mucosal immunity. The results highlight the importance of developing orally and intranasally administered vaccines against SARS-CoV-2.
- Cohen, J. et al. (2022) "Comparison of levels of nasal, salivary, and plasma antibody to SARS-CoV-2 during natural infection and after vaccination", Clinical Infectious Diseases. doi: 10.1093/cid/ciac934. https://academic.oup.com/cid/advance-article/doi/10.1093/cid/ciac934/6884183?login=false
Posted in: Medical Science News | Medical Research News | Disease/Infection News
Tags: Antibodies, Antibody, Assay, Blood, Coronavirus, Coronavirus Disease COVID-19, Healthcare, immunity, Immunoglobulin, Immunoprecipitation, Infectious Diseases, Influenza, Luciferase, Protein, Respiratory, SARS, SARS-CoV-2, Severe Acute Respiratory, Severe Acute Respiratory Syndrome, Spike Protein, Syndrome, Vaccine
.jpg)
Written by
Dr. Chinta Sidharthan
Chinta Sidharthan is a writer based in Bangalore, India. Her academic background is in evolutionary biology and genetics, and she has extensive experience in scientific research, teaching, science writing, and herpetology. Chinta holds a Ph.D. in evolutionary biology from the Indian Institute of Science and is passionate about science education, writing, animals, wildlife, and conservation. For her doctoral research, she explored the origins and diversification of blindsnakes in India, as a part of which she did extensive fieldwork in the jungles of southern India. She has received the Canadian Governor General’s bronze medal and Bangalore University gold medal for academic excellence and published her research in high-impact journals.
Source: Read Full Article