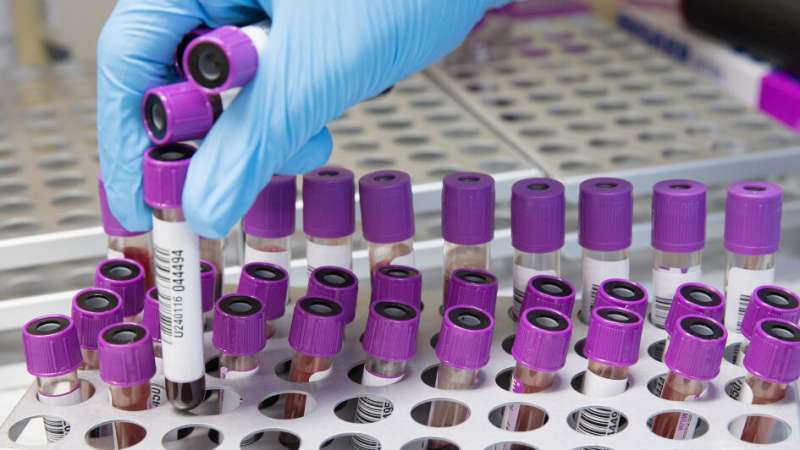
A simple blood test can identify specific genetic mutations in patients’ breast tumors to help guide their treatment and assess how likely patients are to relapse, a study shows.
By allowing clinicians to better understand the genetic characteristics of individual breast cancers, the blood test can be used to guide and adjust treatment without the need to undergo invasive tissue biopsies, which carry risks.
Researchers demonstrated that by using the simple test to analyze traces of tumor DNA circulating in the blood, they were able to identify mutations capable of driving cancer growth and leading to resistance to treatment.
Currently, analysis of tumor DNA found in the blood through simple blood tests—known as liquid biopsies—remains mostly a research tool. This study is a huge step forward in our understanding of how this powerful tool could be used in the clinic routinely to benefit patients with advanced breast cancer.
Looking for HER2, PIK3CA and BRAF gene faults
Scientists at The Institute of Cancer Research, London, and The Royal Marsden NHS Foundation Trust, working in the Breast Cancer Now Toby Robins Research Centre and the Centre for Molecular Pathology, analyzed tumor DNA from blood tests from 800 women with advanced breast cancer who enrolled in the plasmaMATCH trial. They looked for targetable defects in genes such as HER2, PIK3CA and BRAF, which are linked to breast cancer.
One of the benefits of liquid biopsies is that they provide a fuller picture of the genetics of a tumor than conventional, solid tissue biopsies, as they can sample all of a patient’s cancer sites instead of just one small section of a tumor.
By analyzing tumor DNA using liquid biopsies, researchers identified which patients were most likely to have genetic changes in their tumors that could be targeted or could indicate how likely they were to respond to treatment. They also identified a number of new potential therapeutic approaches for advanced breast cancer.
This report from the plasmaMATCH trial, coordinated by the Clinical Trials and Statistics Unit at The Institute of Cancer Research (ICR-CTSU), was published in Nature Communications and funded by Breast Cancer Now and Cancer Research UK through the Stand Up to Cancer campaign.
HER2-positive cancers
Firstly, researchers looked at HER2-positive cancers and found HER2 mutations more commonly in those cancers treated with increasing lines of HER2-targeted therapy—suggesting HER2 mutations evolve through prior treatment and drive resistance. This leads researchers to believe that drugs that target HER2 mutations could be important for treating these patients.
HER2-positive breast cancers produce too much of the growth-promoting protein HER2 and are more likely to come back after treatment than some other types of breast cancer. Around 6,000 women in the UK are diagnosed with this type of cancer in the UK every year.
Hormone receptor-positive, HER2-negative cancers
Scientists also looked at patients with hormone receptor-positive, HER2-negative breast cancer. Those with mutations in both ESR1 and MAPK were identified as a ‘high-risk’ group more likely to develop resistance. Average overall survival was 7.9 months for this group of patients, compared with 18.5 months for patients without the mutations.
They found that among patients with hormone receptor-positive, HER2-negative breast cancer whose tumors had PIK3CA mutations, almost a quarter of patients (47 out of 202) had more than one PIK3CA mutation.
Those with multiple PIK3CA mutations who were treated with fulvestrant saw their disease worsen eight months sooner than patients with a single or no PIK3CA mutation—suggesting an alternative treatment should be considered for these women with multiple PIK3CA gene faults.
In patients with hormone receptor-positive, HER2-negative breast cancer, researchers also identified new BRAF mutations linked to advanced disease—including some BRAF mutations already linked to lung cancer.
Additionally, a small subset of advanced breast cancers (1.1 percent) had ‘microsatellite instability’—a condition that makes cells less capable of correcting mistakes that occur when DNA is copied. Scientists think this group of women could benefit from treatment with immunetherapy antibodies.
These differences in cancer’s genetic makeup mean individual cancers behave differently, so having valuable information about who is likely to develop resistance, and what should be the next treatment to try, would allow clinicians to personalize treatment instead of using a one-size-fits-all approach.
‘A better option than conventional tissue biopsies’
Study leader Professor Nick Turner, professor of molecular oncology at the ICR and head of the Ralph Lauren Centre for Breast Cancer Research at The Royal Marsden, said:
“Our latest plasmaMATCH results identify which genetic alterations are common and most likely to drive breast cancer in different groups of patients, while also shedding light on the processes influencing the development of resistance to treatments.
“We have identified the mutations that breast cancer can acquired to evolve through treatment, helping to advance our understanding of how cancers become resistant to treatment. This will allow us in the future to come up with new strategies to tackle resistance, aiming to improve outcomes for women living with advanced breast cancer.
Source: Read Full Article
