In today’s current era of precision medicine against cancer, research is successfully potentiating and personalizing immunotherapy to unleash the power of the immune system in a greater number of patients to attack disease. Despite such progress, much work is required to better predict those patients who would be most likely benefit from them, and extend their benefits to more patients as well as tumor types—either as monotherapy, or most likely in combination.
“As importantly, we must pursue new therapeutic directions for those patients who are refractory to these novel treatments,” said Alena Gros, principal investigator of VHIO’s Tumor Immunology & Immunotherapy Group, and lead and senior author of a study published open access this week in the Journal of Clinical Investigation.
Carried out in collaboration with Steven A. Rosenberg at the National Cancer Institute (NCI-NIH, Bethesda, U.S.), along with other researchers at the Robert W. Franz Cancer Center (Portland, U.S.) and the Karolinska Institute (Stockholm, Sweden), this study represents an important forward step in alternative treatment approaches for those patients who do not respond to current immunotherapies.
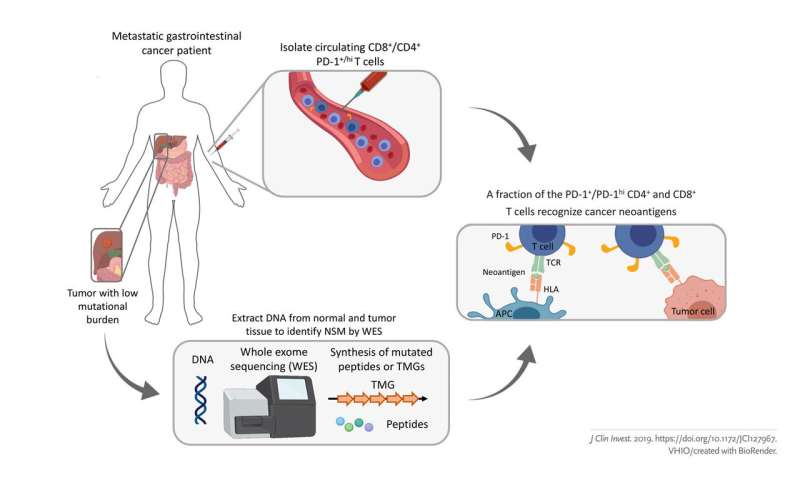
More specifically, those patients with gastrointestinal tumors with low mutational burden, so-called ‘cold’ tumors, constitute a current challenge for immunotherapy. Novel cell therapies based on the administration of killer T cells that can recognize neoantigens have shown promising antitumor activity in a small number of patients with cold tumors.
The new findings promote the development of these treatments for patients with metastatic disease who do not respond to treatment with approved cancer immunotherapies. Additionally, the investigators have described a less invasive, blood-based method to identify, measure and track lymphocytes against neoantigens expressed in advanced gastrointestinal cancers including pancreas, gastroesophageal, bile duct, colon and rectum.
“While we did not expect to find killer T lymphocytes in the blood of these patients with cold tumors of low mutational burden, we have now shown that we can identify and select these cells in blood, which will facilitate and spur the future development of pioneering and personalized cell therapies by liquid biopsy,” noted Alena Gros.
“It is thanks to our strong collaboration with the BBVA Foundation, one of VHIO’s patrons, that we launched our Comprehensive Program of Cancer Immunotherapy & Immunology (CAIMI). This institutional program seeks to advance agents that inhibit checkpoint regulation of the immune system, decipher mechanisms of resistance and response to these therapies, and prioritize the early development of those agents showing most promise. One of our major objectives is to generate novel cell therapies for the more effective treatment of cancer patients,” she concluded.
Source: Read Full Article
