
When Rwandan villager Lillian was diagnosed with cervical cancer, the 30-year-old feared that her life was over. But a new gadget aimed at patients in low-income countries offered her hope.
“The medical diagnosis was very scary; my husband couldn’t believe it,” Lillian—not her real name—told AFP.
“We had heard of people dying of cancer and that it was incurable, so it was a very scary moment.”
Her fears were not unfounded.
Cervical cancer is a notorious “silent killer” of women, but especially so in poor countries that lack affordable treatment and diagnostics.
In Rwanda, it is the most commonly diagnosed cancer, attacking 42 out of every 100,000 women, three times the global average, according to national statistics.
The stigma and fear surrounding the disease and its connection to HIV—a major risk factor for cervical cancer—means many Rwandan women are reluctant even to get tested.
And those who are diagnosed often assume that treatment is out of bounds, unless they live in a major city.
For Lillian, whose village is a three-hour drive east of the capital Kigali, the likelihood of emerging cancer-free, less than four months after diagnosis, seemed like a fantasy.
But in 2020, Rwanda decided to trial a portable device that treats precancerous lesions with heat and can be used in countries with limited access to advanced equipment or facilities.
“The nurse who treated me used a small gadget that looked like a gun. It is uncomfortable but not painful, even when it uses heat to kill the cancer lesions,” Lillian said.
Energy-efficient solution
The so-called C3 thermocoagulator is a pistol-like probe that uses battery power, meaning it can be deployed in remote areas without 24/7 access to electricity.
“The device works by applying heat to the cervix, which causes the abnormal cells to die,” Christine Musabyeyezu, a nurse at Kigali’s Remera health centre, told AFP.
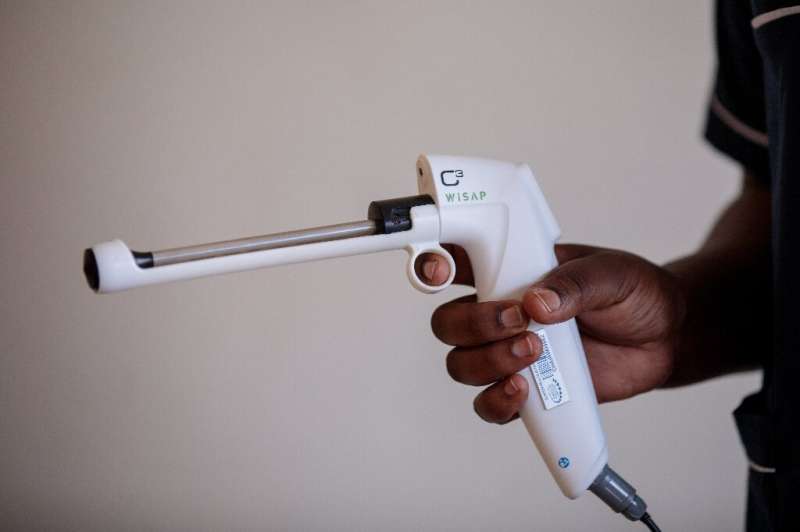
Aimed at being a cost-effective alternative to cryotherapy, the traditional technology used in the treatment of cervical cancer, the device is simple to use, requiring minimal training for health workers, she said.
“At first we relied on cryotherapy to treat cervical cancer lesions, but this method is complicated, expensive and not easily accessible across the country,” Musabyeyezu said.
Cryotherapy, which applies a probe to the cervix to freeze lesions, utilises a lot of energy to ensure that the probe is cold enough.
The thermal devices on the other hand are energy-efficient, offering a week’s worth of use (around 140 treatments) before requiring a recharge.
The gadgets are now at the epicentre of Rwanda’s fight against cervical cancer, particularly in rural areas.
The Central African nation is among seven sub-Saharan countries that have adopted the device, made by a German company, WISAP Medical Technology.
‘Test early, treat early’
Health workers in Rwanda are also hopeful that the success of C3 will go hand-in-hand with a potential breakthrough in diagnostics.
Highly diluted acetic acid—vinegar—has become an established method for spotting pre-cancerous lesions on the cervix, which turn white in the presence of the substance.
However, human interpretation of the test can vary, which is where a mobile app powered by artificial intelligence comes in, boosting accuracy as well as speed.
According to Marisol Touraine, president of the international health agency Unitaid, which is supporting medical trials of the app in Rwanda, more than 300,000 women lose their lives to cervical cancer every year.
The vast majority of these deaths—a staggering 90%—occur in low-income countries “because they were not screened in time, because they were not treated in time,” Touraine told AFP.
The increase in the number of women coming forward to get tested in Rwanda is good news, said nurse Musabyeyezu.
“There is always a queue here of women coming to test for cervical cancer, more than for any other medical tests,” she said.
“This is a good thing because when they test early they can be treated early.”
© 2023 AFP
Source: Read Full Article
