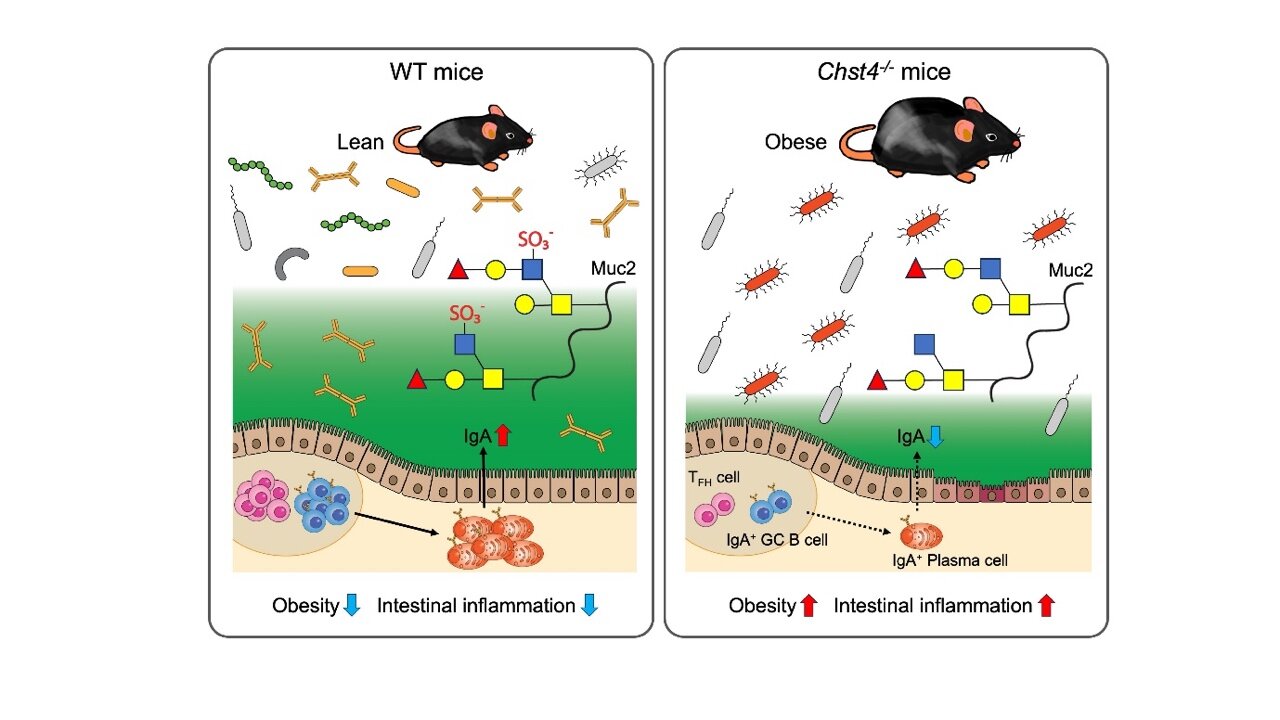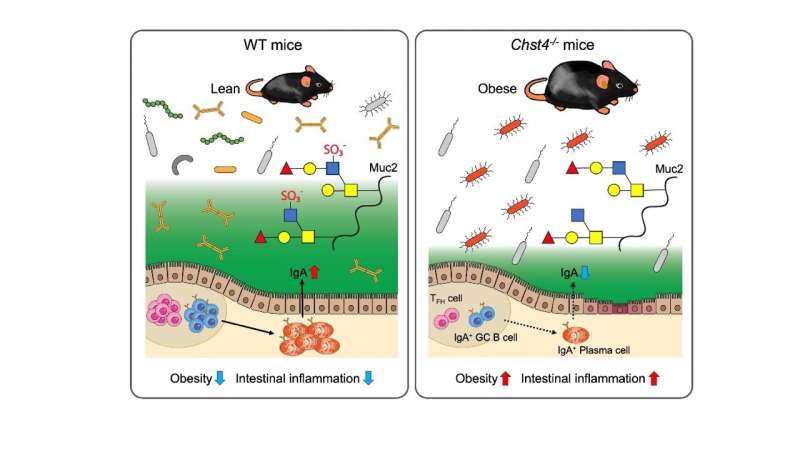
Located in the mucus layer that lines the gastrointestinal tract, mucins—proteins with attached sugar molecules—play a key role in combating bacterial infection and providing a safe haven to friendly gut bacteria through unknown mechanisms. Although mucin dysregulation leads to metabolic disease and intestinal inflammation, the associated mechanism remains largely unknown.
To address this knowledge gap, a team of researchers in Japan explored if the N-acetylglucosamine (GlcNAc)-6-O-sulfation of O-glycans, or the chemical modification of the sugar structures found in mucins, can help combat obesity and intestinal inflammation using a mouse model. This paper was published in JCI Insight.
Initial experiments conducted by the team revealed a significant difference between the intestinal microbiota of regular or “wild type” (WT) mice and Chst4–/– mice that lacked the gene Chst4 for the GlcNAc-6-O-sulfation of mucin glycans. The latter developed obesity and showed vulnerability to both experimental colitis—artificially induced inflammation of the colon—and colitis-associated cancer.
Subsequent experiments revealed several key findings, a major among which was the following: Chst4–/– mice showed reduced fecal levels of immunoglobulin A (IgA), an antibody produced by the immune system that is essential for protecting mucosal surfaces, including the gut, against foreign invasions. Reduced IgA levels in the murine feces, thus, indicate a compromised immune system.
When asked about their results, Professor Hiroto Kawashima from Chiba University’s Graduate School of Pharmaceutical Science, the team’s lead researcher says, “Chst4–/– mice lacking GlcNAc-6-O-sulfation of the mucin O-glycans showed significant weight gain and increased susceptibility to dextran sodium sulfate-induced colitis as well as colitis-associated cancer accompanied by significantly reduced IgA production caused by an impaired T follicular helper cell-mediated IgA response.”
Next, the team found out whether “cohousing” and “microbiota transplantation”—experiments that facilitate the transfer of bacteria between WT and Chst4–/– mice—provided any relief from the observed weight gain and increased susceptibility to colitis. As expected, restoring the healthy gut microbiota in the Chst4–/– rescued the mice from disease and boosted their immune system.
The study authors note that the findings have promising biomedical implications. For instance, enhancing sulfation may provide not only relief against intestinal inflammation but also improve the “barrier function” of epithelial tissues. Epithelial tissues are present in the lining of the skin, gastrointestinal tract, and respiratory tract, among others. They defend against harmful entities by shielding internal body compartments from the external environment.
Although further studies seem necessary, the results may indeed apply not only to obesity and colitis but also to other types of immune-mediated inflammatory diseases, such as nonalcoholic fatty liver disease and nonalcoholic steatohepatitis.
The gut microbiota comprises microorganisms—bacteria, viruses, fungi, protists, archaeans, and other microbes—and related metabolites. Multiple studies acknowledge their close relationship with the immune system. Recently, intestinal microbiota have sparked enormous scientific interest due to their critical roles in protecting the body against many diseases and disorders. The current study confirms earlier findings on friendly gut bacteria while shedding light on a hitherto unknown mechanism involving their regulation by intestinal mucins.
“Collectively, our findings provide insight into the significance of host glycosylation, more specifically GlcNAc-6-O-sulfation on intestinal mucins, in protecting against obesity and intestinal inflammation via regulation of the gut microbiota,” concludes first author Hirohito Abo from the Graduate School of Pharmaceutical Sciences, Chiba University.
More information:
Hirohito Abo et al, N-acetylglucosamine-6-O sulfation on intestinal mucins prevents obesity and intestinal inflammation by regulating gut microbiota, JCI Insight (2023). DOI: 10.1172/jci.insight.165944
Journal information:
JCI Insight
Source: Read Full Article