BOSTON ― The use of carbon dioxide (CO2) laser excision therapy for hidradenitis suppurativa (HS) is not associated with an increased risk for the development of keloids, new research shows.
“With keloids disproportionately affecting Black and other skin of color patients, denying treatment on a notion that lacks evidentiary support further potentiates the health disparities experienced by these marginalized groups,” the researchers reported at the Annual Meeting of the Skin of Color Society Scientific Symposium (SOCS) 2022. In their retrospective study of 129 patients with HS treated with CO2 laser, “there were no cases of keloid formation,” they say.
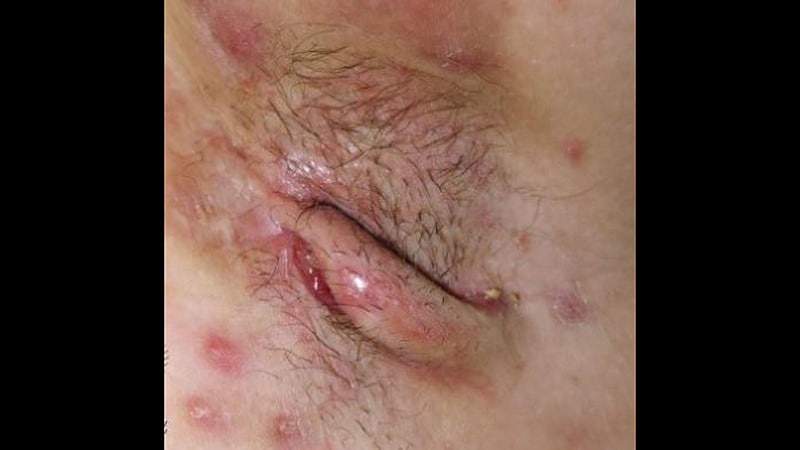
HS, a potentially debilitating chronic inflammatory condition that involves painful nodules, boils, and abscesses, is often refractory to standard treatment. CO2 laser excision therapy has yielded favorable outcomes in some studies.
Although CO2 laser therapy is also used to treat keloids, some clinicians hesitate to use this treatment in these patients because of concerns that its use for treating HS could trigger the development of keloids.
“Many patients come in telling us they were denied [CO2 laser] surgery due to keloids,” senior author Iltefat Hamzavi, MD, a senior staff physician in the Department of Dermatology at the Henry Ford Health System, in Detroit, Michigan, told Medscape Medical News.
Although patients with HS are commonly treated with CO2 laser excision in his department, this treatment approach “is underused nationally,” he said.
“Of note, the sinus tunnels of hidradenitis suppurativa can look like keloids, so this might drive surgeons away from treating [those] lesions,” Hamzavi said.
To further evaluate the risk of developing keloids with the treatment, Hamzavi and his colleagues conducted a retrospective review of 129 patients with HS treated at Henry Ford who had undergone follicular destruction with CO2 laser between 2014 and 2021; 102 (79%) patients were female. The mean age was about 38 years (range, 15 to 78 years).
Of the patients, almost half were Black, almost 40% were White, 5% were Asian, and 3% were of unknown ethnicity.
Medical records of nine patients included diagnoses of keloids or hypertrophic scars. Further review indicated that none of the diagnoses were for keloids but were for hypertrophic scars, hypertrophic granulation tissue, an HS nodule, or contracture scar, the authors report.
“While the emergence of hypertrophic scars, hypertrophic granulation tissue, and scar contracture following CO2 laser excision therapy for hidradenitis suppurativa has been documented in the literature, existing evidence does not support post-operative keloid formation,” the authors conclude.
Because healing time with CO2 laser treatment is prolonged and there is an increase in risk of adverse events, Hamzavi underscored that “safety protocols for CO2 lasers should be followed, and wound prep instructions should be provided along with counseling on healing times.”
Regarding patient selection, he noted that “the disease should be medically stable with reduction in drainage to help control postop bleeding risk.”
The findings of the study are supported by a recent systematic review that compared outcomes and adverse effects of treatment with ablative laser therapies with nonablative lasers for skin resurfacing. The review included 34 studies and involved 1093 patients. The conditions that were treated ranged from photodamage and acne scars to HS and posttraumatic scarring from basal cell carcinoma excision.
That review found that overall, rates of adverse events were higher with nonablative therapies (12.2%, 31 events) in comparison with ablative laser therapy, such as with CO2 laser (8.28%, 81 events). In addition, when transient events were excluded, ablative lasers were associated with fewer complications overall in comparison with nonablative lasers (2.56% vs 7.48%).
The authors conclude, “It is our hope that this study will facilitate continued research in this domain in an effort to combat these inequities and improve access to CO2 excision or standardized excisional therapy for hidradenitis suppurativa treatment.”
Hamzavi and the other authors have disclosed no relevant financial relationships.
Annual Meeting of the Skin of Color Society Scientific Symposium (SOCS) 2022: Poster 49. Presented March 24, 2022.
For more news, follow Medscape on Facebook, Twitter, Instagram, and YouTube.
Source: Read Full Article